Author’s Corner
In his white paper, Roopesh Shetty, Vice President of Strategic Accounts, examines common causes of improper payment error categories and how to avoid them. In particular, Roopesh details how Vee Healthtek takes a unique approach to correcting errors on the CPT level.
Please click on the video to the right to learn more about the author, his paper’s key points, and his interest in RPA.
To discuss this white paper further, please contact Roopesh using his information provided at the bottom of the page.
According to the 2019 statistics released by CMS for “Common Causes of Improper Payment Error Categories”:
- 59.5% of cases are due to insufficient documentation
- 18.7% of cases are caused by medical necessity
- 13.7% of cases result from incorrect coding
- 8.2% of cases occur because of no documentation and other categories
The data is highlighting the top reasons for revenue leakage. Based on the above statistics, almost 92% of the error rate is due to clinical, documentation, and coding-related issues. It is an eye-opener for most hospitals and physician organizations needing to focus their attention on clinical and coding parts of the RCM process to improve their compliance and reimbursement.
Vee Healthtek’s consulting teams provide a unique approach and solutions by helping hospitals and physician organizations develop overall coding and documentation compliance, thereby identifying opportunities to improve their outcome.
An East coast-based hospital was under tremendous financial pressure because of constant revenue leakage and increasing overheads. The physician group, with more than 300 doctors onboard, were taking care of patients and doing their coding. While physicians are good at treating patients, most struggle or have a limited understanding of coding. Physicians tend to pick codes based on their experience and assessment of the patient’s situation that they may or may not have captured in the documentation. It can potentially open up a compliance issue or lost revenue.
The client had seven or eight coders who were primarily responsible for clearing coding-related edits to release the claims. The external audit conducted by the client showed poor quality results.
However, the audit company provided no data or intelligence that would help the client identify the root cause of the problem. Vee Healthtek provided a multi-step approach, keeping in mind the client’s budgetary limitations and focusing on improving the effectiveness of the process.
Vee Healthtek used the following approach and potential solution:
Approach:
- Conduct sample audit based on surgery and other chart types for the last three months
- Share audit results with root cause analysis
- Coding issues
- Documentation issues
- Missed opportunities
- Physicians education opportunities
Solution:
- Conduct extensive ongoing audit for several months
- Educate physicians and coders based on audit findings
- Improve clinical documentation education and coaching
- Review medical necessity and denials
- Create edits to reduce denials
- Perform coding services as an ongoing solution for complex chart types
The initial sample audit conducted at no cost to the client was provided by Vee Healthtek to identify minimum committed improvement opportunities. If the audit results did not show significant ROI, the client would continue with their process. However, if Vee Healthtek could demonstrate substantial opportunities and ROI, the client would consider implementing the recommended solutions.
Initial audit results shared by Vee Healthtek with error categorization and Revenue Impact:
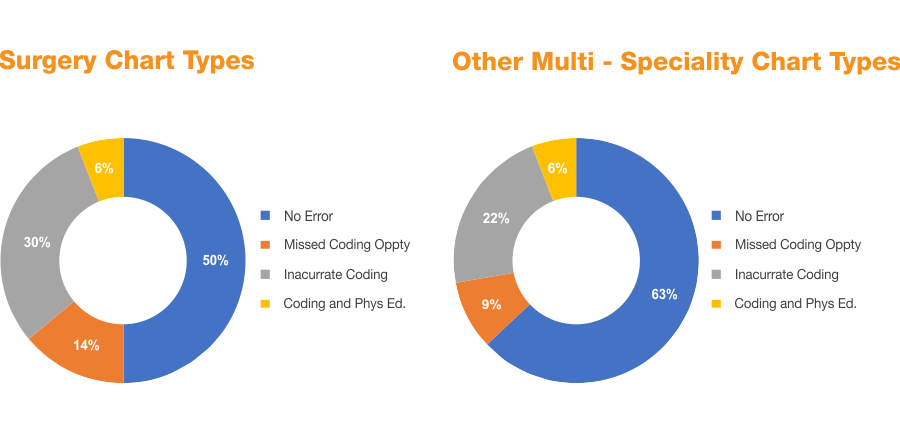
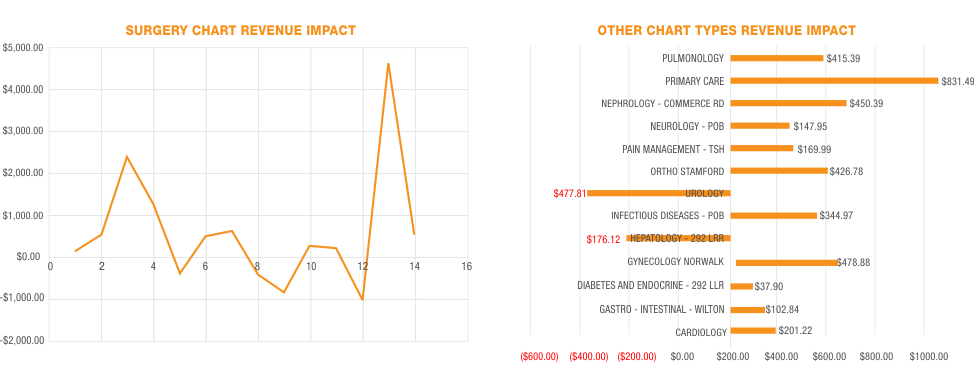
Surgery/Complex coding audit:
- Almost 50% of the errors on the CPT level are due to inappropriate coding in surgery claims.
- In approximately 8% of the claims, there was non-compliant coding that resulted in excess payment to the client.
- Approximately 6% of the claims indicated there is an opportunity to improve the documentation through physician education.
- The audit identified almost $10,000 of missed coding opportunity (lost revenue) that represent only 2.5% of the average monthly surgical case volume.
- If this finding is extrapolated out to 100% of the monthly surgery claims, there is approximately $400,000 of lost revenue opportunity each month.
Multispecialty:
- On the claim level, overall coding accuracy was 75% for multispecialty cases.
- In approximately 5% of the claims, there was non-compliant coding that resulted in excess payment to the client.
- About 5% of the claims indicated there is an opportunity to improve the documentation through physician education.
- The audit Identified almost $3,000 of missed coding opportunities (lost revenue) that represented only 2% of the average monthly non-surgical multispecialty claim volume.
- If this finding is extrapolated out to 100% of the monthly multispecialty claims, it results in approximately $200,000 of lost revenue opportunity each month.
During the pandemic, most hospitals saw a significant drop in volume and revenue. It is critical for hospitals to improve collections and reduce denials through process efficiency and identify opportunities to boost revenue by remaining compliant.
Vee Healthtek's consulting engagement does not stop with solution recommendations. Our team of expert physicians, nurses, and certified coders work with clients to implement solutions and ensure success through coding education, audit plans, CDI opportunities, physician education, and denial management.

